The Neuroimmunological Architecture of Anxiety: How Brain Inflammation Creates Physical Symptoms

The Neuroimmunological Architecture of Anxiety: How Brain Inflammation Can Shape Physical Symptoms
Understanding the neural mechanisms behind why anxiety can feel so physical
If your anxiety comes with chest pressure, gut churn, or aching muscles you are not imagining it. Research links anxiety with measurable immune signaling in the body, and stress can influence brain barriers and circuits that regulate bodily sensations. The strength of evidence varies by topic, so this page focuses on what is well supported and what is emerging.
Think of anxiety as both a feeling and a shift in body state. Brain regions that track threat also coordinate breathing, heart rhythm, gut motility, and pain sensitivity. Immune signals can interact with these systems, which helps explain why anxiety often feels physical.
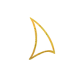
What We Know With Confidence
Immune Pathways Often Discussed
Interleukin 6, TNF alpha, and CRP
These markers are frequently elevated with chronic stress in population studies. In generalized anxiety disorder specifically, meta analysis suggests group differences at the peripheral level, but not uniformly across all studies. Interpretation requires caution because lifestyle, sleep, and comorbid conditions influence these markers.
Kynurenine Pathway
Inflammation can shift tryptophan metabolism away from serotonin toward kynurenine metabolites. This mechanism is best established in depression and sickness behavior, with mixed but growing relevance for anxiety. Nat Rev Immunol overview; systematic review.
What About Brain Imaging and “Neuroinflammation”?
Positron emission tomography using TSPO ligands can index glial activation in some disorders. Findings across psychiatric conditions are mixed, and anxiety specific PET results are limited. Some studies report no clear association between TSPO signal and anxiety measures, while others focus on depression or PTSD. It is more accurate to say that neuroimmune interactions are plausible and under active study rather than proven universally elevated in anxiety. Review 2019; Dahoun et al. 2019; Review 2025.

Turn insight into a practical plan
Learn how breathing pace, sleep regularity, and anti inflammatory patterns can reduce symptom intensity.
Work with our Anxiety SpecialistPractical Steps With Low Risk and Good Support
- Slow breathing near 6 breaths per minute for 2 to 5 minutes. Improves vagal tone and symptom control for many people.
- Sleep protection with a consistent window and darker, cooler nights.
- Dietary pattern rich in omega 3 fish, olive oil, pulses, and colorful plants. This supports lower inflammatory tone.
- Gentle aerobic movement most days to stabilize autonomic balance.
- Professional support if symptoms are frequent, severe, or function limiting.
Frequently Asked Questions
Some PET tracers can reflect glial activation, but anxiety specific evidence is limited and mixed. Most TSPO PET findings focus on depression or PTSD, and some studies report no association with anxiety scores. These tools are valuable for research rather than diagnosis. See 2019 review and Dahoun 2019.
Acute stress can alter autonomic tone within seconds and can shift immune signaling over hours to days. In chronic stress models, barrier and cytokine changes emerge over days to weeks. Human peripheral markers can fluctuate with sleep, infection, and metabolic state, so single readings need context.
Estrogen decline reduces anti inflammatory buffering and can change sleep, thermoregulation, and autonomic balance. Reviews describe higher pro inflammatory signaling post menopause and mechanisms for estrogen immune regulation.
Related Research Articles
Why Your Anxiety Creates Real Physical Pain
How immune signaling can influence body sensations during anxiety, with practical steps.
Why Anxiety Can Feel Worse After 40
Hormonal and sleep changes that alter stress perception and recovery.
Sleep, Anxiety, and Inflammation
How sleep stabilizes autonomic function and inflammatory tone.
