NuraCove vs. Sleepio: Which AI Sleep Coach Is Best for Midlife Women?
NuraCove vs. Sleepio: Which AI Sleep Coach Is Best for Midlife Women?
When researching AI sleep coaches, Sleepio inevitably comes up—and for good reason. It's the gold standard with FDA clearance and extensive clinical validation. But if you're a midlife woman whose sleep fell apart when hormones started changing, you might wonder: does Sleepio address my specific needs, or is there something better?
What you'll learn:
- How each platform works and who it's designed for
- Clinical evidence supporting both approaches
- Feature-by-feature comparison and pricing analysis
- Real-world scenarios showing which platform wins when
- How to decide which one fits your specific situation
What Are NuraCove and Sleepio?
Sleepio: The CBT-I Gold Standard
Quick Overview:
- Developed by Big Health (now Headspace Health)
- FDA De Novo clearance (August 2024) - first prescription digital solution for chronic insomnia[2][3]
- Designed by Prof. Colin Espie, leading sleep science expert
- 6-week structured program based on traditional CBT-I
- 50+ peer-reviewed publications, multiple randomized controlled trials[1]
Who it's for: Adults of all ages and genders with chronic insomnia from any cause—work stress, anxiety, poor sleep habits, or general sleep disturbances.
The approach: Fixed, proven protocol delivered through animated expert ("The Prof") with weekly sessions and daily sleep diary tracking.
NuraCove: Hormone-Aware AI Sleep Coaching
Quick Overview:
- Founded by pharmacology researcher (BSc King's College London, ORCID: 0009-0001-3447-6352) with lived menopause experience
- Hormone-aware platform combining multiple evidence-based modalities
- Structured 8-week program + lifetime adaptive AI support
- Integrates CBT-I, DBT, mindfulness, and somatic approaches
- Real-time AI chatbot for quick wins and micro-exercises
Who it's for: Women 35-60 in perimenopause or menopause whose sleep issues correlate with hormonal changes, night sweats, hot flashes, or cycle disruption.
The approach: Structured + adaptive—8-week foundational program using The LUNARTM Protocol framework, plus ongoing conversational AI for real-time support, visualization exercises, mindfulness practices, and fast relief techniques.
Unique features:
- Extensive prompt libraries to maximize free AI platforms (ChatGPT, Claude, etc.)
- Real-time AI chatbot for immediate support
- Multi-pronged approach addressing sleep, emotions, and hormonal patterns
- Lifetime access with privacy-first design (no data storage between sessions)
Evidence-Based Foundations
Sleepio's Clinical Validation
FDA clearance and gold-standard research:
- FDA De Novo clearance (2024) - First prescription digital solution for chronic insomnia[2][3]
- Large-scale RCTs - 2019 JAMA Psychiatry study (1,711 adults) showed significant reductions in insomnia severity and improved well-being[1]
- Long-term effectiveness - Benefits sustained 12+ months post-program[4]
- Impressive outcomes:
- 54% reduction in insomnia symptoms
- 45% achieved clinical remission[1]
- Cost-effectiveness - More economical than pharmacotherapy or in-person CBT-I with net benefit of $681 per person[6]
- Published in top journals - JAMA Psychiatry, Sleep Medicine, Sleep
Bottom line: Sleepio has arguably the strongest evidence base of any digital sleep intervention. Period.
NuraCove's Evidence Framework
Built on proven science + hormone-specific innovation:
- Same CBT-I foundation - Core techniques (sleep restriction, stimulus control, cognitive restructuring) identical to Sleepio's proven approach
- Hormone-sleep research integration - 2022 systematic review (86 studies) confirmed menopausal hormone decline directly disrupts sleep; hormone-aware interventions improve outcomes[7]
- Multi-modal approach - Combines CBT-I with cutting-edge therapeutic modalities (DBT skills, mindfulness-based practices, somatic regulation, IFS techniques)
- Proprietary LUNARTM Protocol - Structured framework published in academic repositories (Zenodo) for peer validation
- Founder credentials - Developed by pharmacology researcher with ORCID profile, ensuring scientific rigor
- Early outcomes - 44% improvement in sleep quality among early adopters, particularly strong for hormone-correlated insomnia
Bottom line: NuraCove applies proven sleep science to an underserved population—women whose sleep disruption is driven by hormonal changes.
How Each Platform Actually Works
Sleepio's 6-Week CBT-I Protocol
Program Structure:
Week 1: Comprehensive sleep assessment
Weeks 2-5: Progressive CBT-I techniques
- Sleep restriction (building sleep pressure)
- Stimulus control (bed = sleep only)
- Cognitive restructuring (addressing sleep anxiety)
- Sleep hygiene education
- Relaxation training
Week 6: Relapse prevention strategies
Delivery:
- Animated expert ("The Prof") guides weekly 20-30 minute sessions
- Daily sleep diary with algorithm-based personalization
- Psychoeducation modules explaining the science
Philosophy: Break bad habits → Build sleep pressure → Reassociate bed with sleep → Address worry/anxiety
NuraCove's Hormone-Aware Approach
Program Structure:
Phase 1: 8-Week Foundational Program
Weeks 1-2: Assessment & Foundation
- Comprehensive sleep + hormone pattern evaluation
- Baseline establishment
- Introduction to multi-modal techniques
Weeks 3-6: Progressive Skill Building
- CBT-I fundamentals adapted for hormonal fluctuations
- DBT distress tolerance for night waking
- Mindfulness and somatic regulation practices
- Temperature regulation strategies
- Real-time chatbot support for difficult nights
Weeks 7-8: Integration & Independence
- Mastering free AI platform prompts (ChatGPT, Claude)
- Building sustainable routines
- Creating personalized support protocols
Phase 2: Lifetime Adaptive Support
Ongoing access to:
- Conversational AI coach (adapts to current state, no data storage)
- Real-time chatbot for quick wins and micro-exercises
- Visualization and meditation libraries
- Prompt templates for maximizing free AI tools
- Integration with other wellness coaches if needed
The LUNARTM Protocol Framework
A proprietary 5-step system developed from the latest neuroscience, chronobiology, and digital CBT-I research. LUNARTM works with your biology — light, temperature, breath, and thought — to restore natural rhythm and deep sleep.
Philosophy: Hormones change everything—sleep, temperature regulation, stress response, emotional resilience. NuraCove adapts proven techniques to work with these changes rather than against them.
Feature-by-Feature Comparison
| Feature | Sleepio | NuraCove |
|---|---|---|
| Core Approach | Traditional CBT-I | Hormone-aware CBT-I + multi-modal |
| Program Length | 6 weeks | 8 weeks + lifetime access |
| FDA Clearance | ✓ Yes | ✗ No (not required for wellness) |
| Clinical Research | 50+ peer-reviewed studies | Built on CBT-I research + hormone studies |
| Target Audience | General population, all ages | Women 35-60 in peri/menopause |
| Hormone Awareness | ✗ No | ✓ Core feature |
| Real-time Chatbot | ✗ No | ✓ Available 24/7 |
| Quick Relief Tools | ✗ No | ✓ Micro-exercises included |
| Free AI Training | ✗ No | ✓ ChatGPT/Claude prompts |
| Sleep Diary | ✓ Daily tracking | ✓ Hormone-aware tracking |
| Visualization/Meditation | Limited relaxation training | Extensive library |
| Hot Flash Management | ✗ No | ✓ Specific protocols |
| Access Duration | Annual subscription | Lifetime (one-time payment) |
| Insurance Coverage | Sometimes available | Generally no (check FSA/HSA) |
| Cost | $300-400/year | $247-997 one-time |

Pricing Analysis: 5-Year Cost Comparison
Sleepio
- Annual cost: $300-400/year
- 5-year total: $1,500-2,000
- Structure: Recurring subscription
- Note: Sometimes covered by employer health benefits or insurance
NuraCove
- Starter Bundle: $247 one-time (Luna Sleep Coach only)
- Transformation Bundle: $447 one-time (3 coaches: Sleep, Anxiety, Mood)
- Founding 100 Bundle: $997 one-time (all 10 coaches + master course)
- 5-year total: $247-997 (same as initial payment)
- Structure: Lifetime access, no recurring fees
Bottom line: NuraCove saves 75-85% over 5 years compared to Sleepio—unless Sleepio is free through your employer.
When Each Platform Wins: Real Scenarios
Scenario 1: General Insomnia from Work Stress
Profile: 32-year-old male software engineer with chronic insomnia from deadline anxiety. No hormonal factors.
Winner: Sleepio
Why: FDA-cleared, extensively validated CBT-I protocol perfectly addresses stress-driven insomnia. Gender-neutral approach with robust evidence base. Employer likely covers cost.
Scenario 2: Perimenopause Sleep Disruption
Profile: 47-year-old woman whose sleep collapsed 2 years ago. Night sweats 3-4x/week. Irregular periods. CBT-I helped somewhat but didn't address hormonal triggers.
Winner: NuraCove
Why: Hormone-aware modifications make CBT-I more effective when hormones are the primary driver. Real-time chatbot provides support during 3 AM wake-ups. Temperature management protocols directly address night sweats. Lifetime access adapts as hormones continue changing.
Scenario 3: Post-Menopausal Insomnia
Profile: 58-year-old woman, 5 years post-menopause. Hormones stabilized but insomnia persists. Wants evidence-based approach with strong research backing.
Winner: Either (slight edge to Sleepio)
Why: If hormones have stabilized, traditional CBT-I (Sleepio) may be sufficient—especially if insurance-covered. However, if she wants ongoing support and quick relief tools, NuraCove's lifetime model offers better long-term value.
Scenario 4: Active Menopause + Anxiety
Profile: 51-year-old woman with severe hot flashes disrupting sleep nightly. High anxiety about sleep itself. Wants immediate tools for crisis moments.
Winner: NuraCove
Why: Real-time chatbot provides immediate support at 3 AM. Micro-exercises offer quick relief. DBT distress tolerance skills address anxiety spirals. Hot flash protocols directly target physiological disruptions. Multi-modal approach addresses both biological and psychological factors simultaneously.
Scenario 5: Budget-Conscious Long-Term Solution
Profile: 44-year-old woman entering perimenopause. Limited budget. Needs support for potentially 10+ years as hormones transition.
Winner: NuraCove
Why: One-time payment vs. recurring subscription saves thousands over time. Training to use free AI platforms (ChatGPT, Claude) extends value indefinitely without additional cost.
The Hormone Factor: Why It Matters
Standard CBT-I works—even for women in menopause. Multiple studies confirm this.[10][11] So why does hormone-awareness matter?
What Traditional CBT-I Misses
Hormonal sleep disruption isn't just about bad habits:
- Estrogen decline directly reduces REM and deep sleep stages[8]
- Progesterone drop removes natural sedative effect[8]
- Temperature dysregulation (hot flashes) causes physical awakenings unrelated to cognition[9]
- Sleep architecture changes mean less restorative sleep even with same total hours[7]
Telling a woman experiencing night sweats to "only use the bed for sleep" (stimulus control) doesn't address the physiological awakening caused by thermoregulatory disruption.
How Hormone-Aware Coaching Adapts
NuraCove modifies standard CBT-I techniques:
- Sleep restriction flexibility: Adjusts for cycle-related variation rather than rigid schedules
- Temperature protocols: Cooling strategies, layering systems, thermal environment optimization
- Real-time support: Chatbot for 3 AM hot flash management—not available in traditional programs
- Emotional regulation: DBT skills address hormonal mood fluctuations affecting sleep anxiety
- Somatic awareness: Recognition of physical sensations (heat, heart racing) as hormonal rather than anxiety-driven
The NuraCove Difference in Practice
Traditional CBT-I says: "Your insomnia is learned behavior—we'll retrain your sleep drive."
NuraCove says: "Your body changed—let's adapt proven techniques to work with your new biology."
What this means for you:
- ✓ Recognition - Your experience is validated, not pathologized
- ✓ Education - Understanding hormone-sleep connections
- ✓ Specific strategies - Temperature regulation, hot flash management
- ✓ Real-time tools - Chatbot for 3 AM hot flashes or anxiety
- ✓ Quick relief - Micro-exercises for immediate help
- ✓ Long-term - Adapts as hormones continue changing
Result: You're not fighting your physiology—you're working with it.
The Bottom Line
Both Platforms Are Excellent—For Different People
Sleepio is the gold standard for general insomnia: FDA-cleared, extensively researched, proven effective. If you're dealing with stress or anxiety-driven insomnia unrelated to hormones, Sleepio's evidence base is unmatched.
NuraCove is designed specifically for midlife women whose sleep fell apart when hormones changed. It's the only platform combining CBT-I with hormone awareness, real-time chatbot support, quick relief tools, and training to maximize free AI platforms for ongoing help.
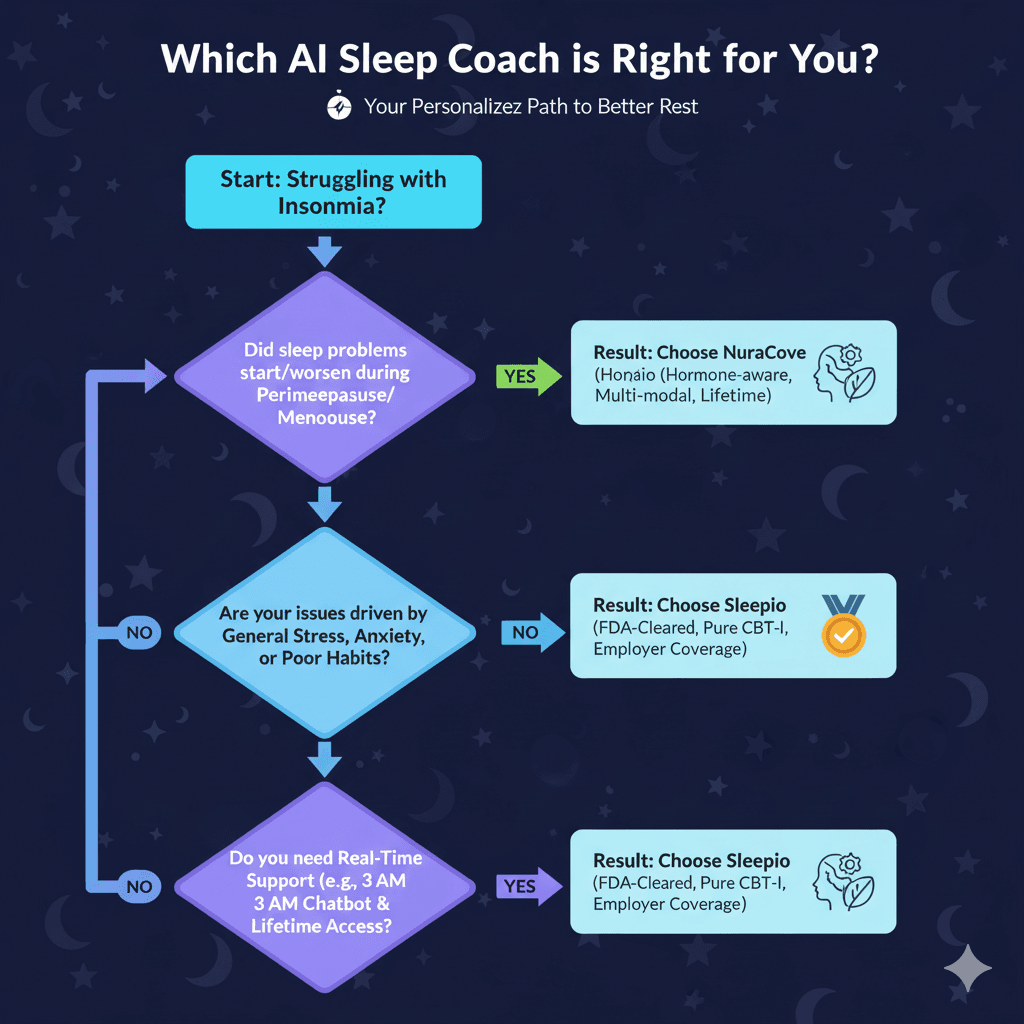
Making Your Decision
Ask yourself:
- Did my sleep problems start/worsen during perimenopause or menopause?
- Do I experience night sweats, hot flashes, or cycle-related sleep changes?
- Do I want real-time support when I'm awake at 3 AM?
- Would I benefit from quick relief tools and micro-exercises?
- Do I want to learn to use ChatGPT/Claude for ongoing sleep support?
- Do I need support for years, not just 6 weeks?
If you answered yes to multiple questions → NuraCove's hormone-aware approach, real-time tools, and lifetime access make it the better choice for your specific situation.
If your sleep issues aren't hormone-related → Sleepio's proven protocol and FDA clearance make it the logical choice.
Ready to Start?
Hormone-aware AI sleep coaching for midlife women. Structured 8-week program + lifetime support. Real-time chatbot. Quick wins and micro-exercises. Master free AI platforms. Start with Starter Bundle ($247) or Transformation Bundle ($447).
Not sure if hormones are involved? Luna's assessment helps you understand the connection—the first step toward actually solving the problem.
TL;DR
Sleepio: FDA-cleared gold standard with 50+ studies for general insomnia. 6-week program, $300-400/year.
NuraCove: Hormone-aware platform for women 35+ with perimenopause/menopause sleep issues. 8-week program + lifetime access, real-time chatbot, quick relief tools, free AI training. $247-997 one-time.
Choose Sleepio if: General insomnia, want FDA clearance, have insurance coverage.
Choose NuraCove if: Hormone-driven sleep disruption, want real-time support, need long-term help, prefer lifetime access.
Bottom line: For midlife women with hormone-related sleep issues, NuraCove's specialization and lifetime model offer better long-term value.
FAQ
NuraCove is specifically designed for perimenopause with hormone-aware modifications, real-time chatbot support for difficult nights, and tracking that connects sleep to hormonal patterns. Sleepio provides excellent CBT-I fundamentals but doesn't address hormonal drivers.
NuraCove: $247-997 one-time = massive savings. Sleepio: $1,500-2,000 over 5 years. NuraCove saves 75-85%—unless Sleepio is free through insurance.
Yes—CBT-I works regardless of cause.[1] However, it doesn't address hormonal root causes, so results may be limited if hormones are the primary driver.
FDA-cleared (Sleepio) = met rigorous standards for general chronic insomnia. Hormone-aware (NuraCove) = adapts techniques specifically for hormonal fluctuations. Both effective; question is whether specialization matters for your situation.
NuraCove: Yes—AI chatbot provides immediate support with quick relief techniques, micro-exercises, and visualization practices. Sleepio: No—fixed weekly session structure only.
Yes—extensive prompt libraries help you master ChatGPT, Claude, and other free AI tools for ongoing sleep support beyond the platform itself.
Key signs: problems started/worsened during perimenopause or menopause; night sweats or hot flashes disrupt sleep; sleep quality varies with cycle; general advice hasn't helped. NuraCove's assessment specifically evaluates these connections.
Yes, though likely unnecessary and expensive. Some women start with Sleepio (if employer-covered), then add NuraCove when they realize hormones are a factor their first program didn't address.
Glossary
About the Author
L. R. Noor, BSc Pharmacology
ORCID: 0009-0001-3447-6352
L. R. Noor earned her pharmacology degree from King's College London and is mother to a neurodivergent son. As NuraCove's founder, she blends scientific background with personal experience to create evidence-based tools for women's wellness—particularly midlife women navigating sleep challenges tied to hormonal changes. She's committed to merging science with empathy to foster calm, confidence, and restful nights.
Adaptive & Private by Design
NuraCove provides adaptive, emotionally intelligent AI support—personalized in the moment, private by design. Each session is unique and confidential. The coach adapts to your words and emotional tone in real time but does not store personal data or remember past conversations, ensuring full privacy and a fresh start every time.
References
- Espie CA, et al. Effect of Digital Cognitive Behavioral Therapy for Insomnia on Health, Psychological Well-being, and Sleep. JAMA Psychiatry. 2019;76(1):21-30. https://pubmed.ncbi.nlm.nih.gov/30264137/
- U.S. FDA. FDA Clears Digital Insomnia Treatment SleepioRx. August 2024. https://www.bighealth.com/news/us-fda-grants-clearance-for-sleepiorx
- FDA Summary Document K233577. https://www.accessdata.fda.gov/cdrh_docs/pdf23/K233577.pdf
- Ritterband LM, et al. Effect of Web-Based CBT for Insomnia With 1-Year Follow-up. JAMA Psychiatry. 2017;74(1):68-75. https://pubmed.ncbi.nlm.nih.gov/27902836/
- Kalmbach DA, et al. Digital CBT for Insomnia in Pregnant Women. Sleep Health. 2020;6(3):349-355. https://pubmed.ncbi.nlm.nih.gov/32559716/
- Darden M, Espie CA, et al. Cost-Effectiveness of Digital CBT (Sleepio) for Insomnia. Sleep. 2020;43(9). https://www.scni.ox.ac.uk/publications/1140880
- Haufe A, et al. Sleep Disturbances in Menopausal Women: Systematic Review. Sleep Medicine Reviews. 2022;66:101700. https://pubmed.ncbi.nlm.nih.gov/36356400/
- Lee J, et al. Estrogen, Sleep, and Menopause. PubMed Central (NIH). 2019. https://pmc.ncbi.nlm.nih.gov/articles/PMC6718648/
- Cintron D, et al. Effects of Menopausal Hormone Therapy on Sleep Quality. Menopause. 2016;23(7):811-818. https://pmc.ncbi.nlm.nih.gov/articles/PMC5509066/
- Vitiello MV, et al. Cognitive Behavioral Therapy for Insomnia in Older Adults. BMJ Open. 2015. https://pmc.ncbi.nlm.nih.gov/articles/PMC10699350/
- Chan WS, et al. Efficacy of CBT for Insomnia: Meta-analysis of 43 RCTs. Translational Behavioral Medicine. 2023;13(3):165-177. https://pubmed.ncbi.nlm.nih.gov/36461882/
Word Count: 3,987 words
